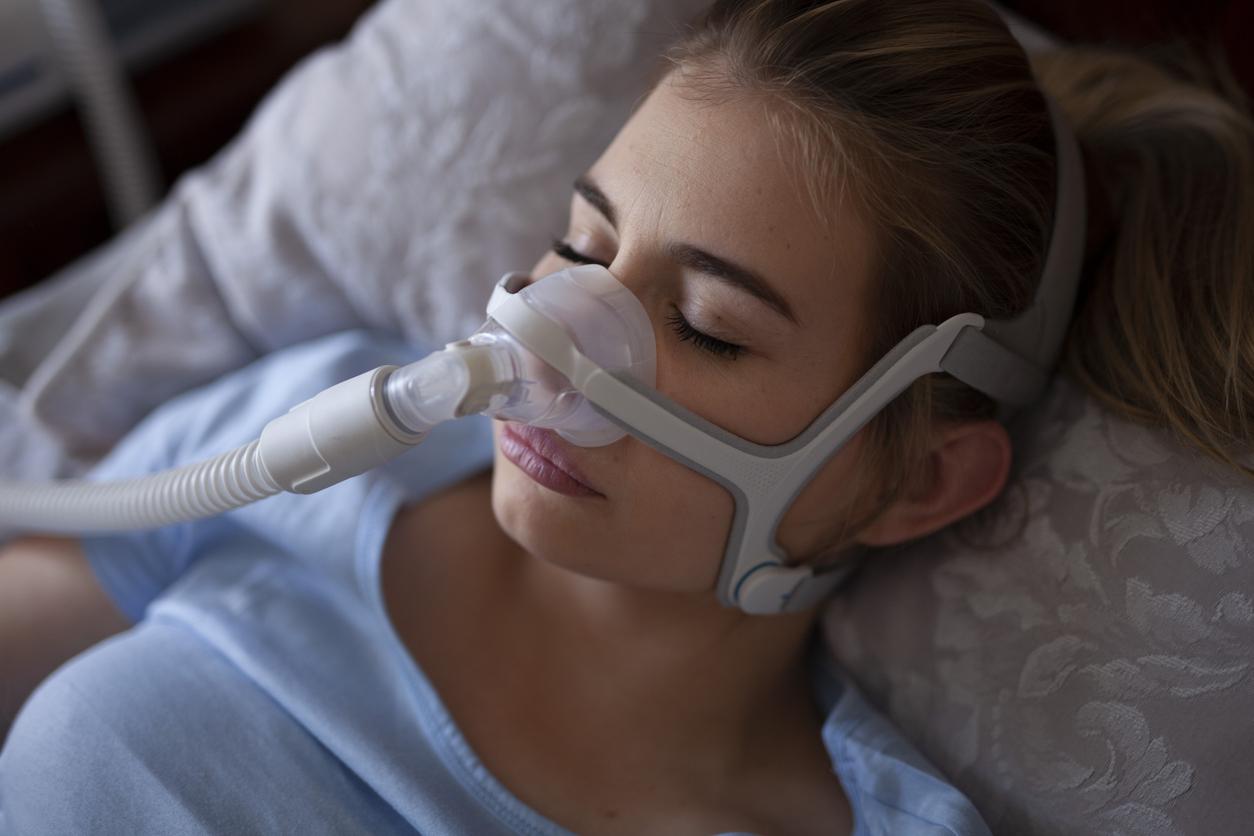
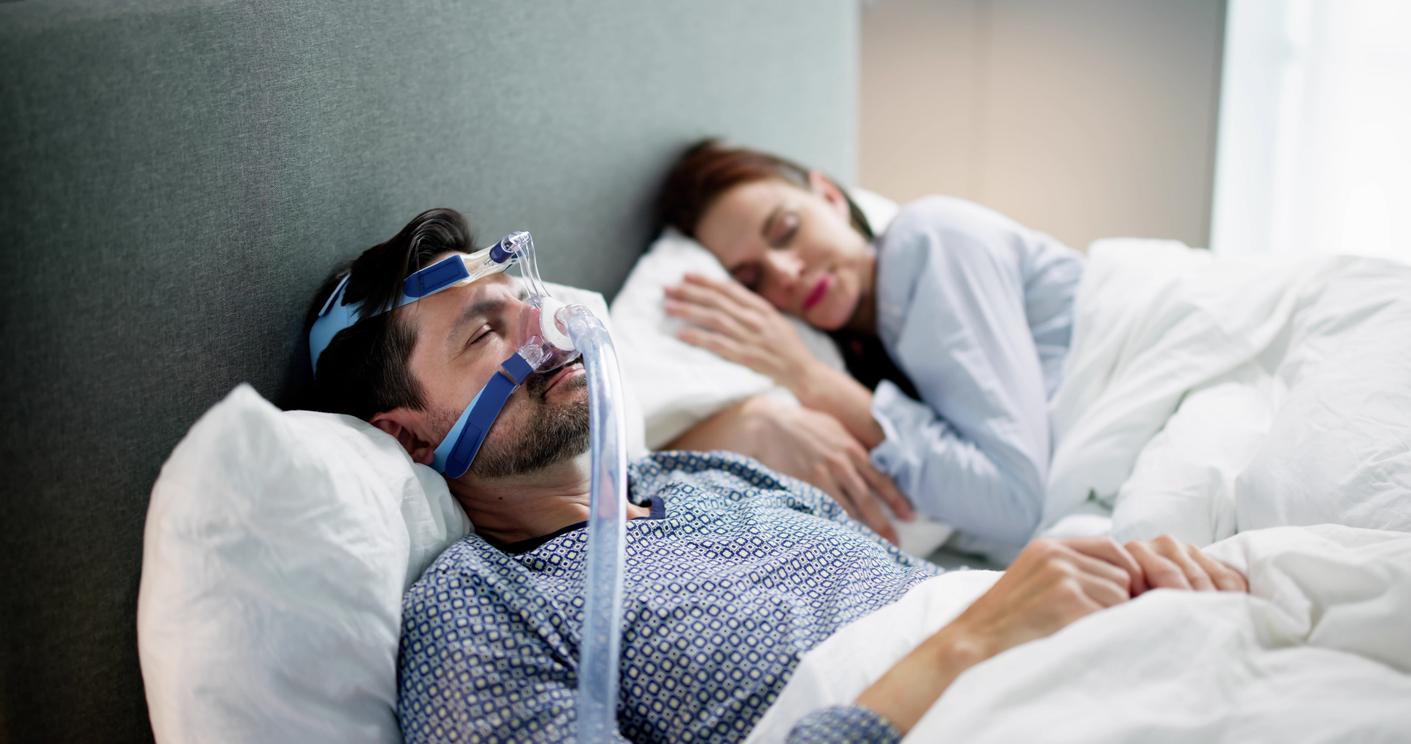
Applications and connected objects to monitor the quality of sleep are multiplying. While some of these devices can help solve insomnia or other disorders, others do not provide sufficient precision to direct towards a diagnosis or treatment. Update with cardiologist Pierre Escourrou.

– Why Doctor: What are the connected devices or objects that can be used to control or improve sleep?
Professor Pierre Escourrou : There are a large number of them, hitherto rather oriented towards “well-being” and which, for some, have no obvious medical application. First there are smartphone applications for monitoring sleep, objects worn by the patient, watches or rings, and contactless objects. The applications use two types of signals, actimetry -sleep and wakefulness phases- and variations in movements and sounds, the objects worn record movements and heart rate and there are also headbands or masks on the eyes which can collect encephalographic data.
– What can we learn from these data about sleep?
They provide information on the waking and sleeping phases and make it possible to distinguish the different stages of sleep that appear during the night, light sleep, deep slow-wave sleep and paradoxical sleep. This is interesting because it can help to know the quality of sleep, especially for deep slow-wave sleep which is the restorative part of sleep.
– Can these data be interpreted by the patient himself or only by a doctor?
To interpret them, it is necessary to know the normal values and the meaning of the different variations. This has no interest for the patient himself because it is not related to his feelings. The most important element is the duration of actual sleep compared to the time spent in bed, which is called sleep efficiency. It is a basic parameter which is essential for the patient and of course for the doctor who monitors him.
– How can doctors use this data?
At this time, there is insufficient scientific validation to use sleep stage data. But for the distinction between sleep and wake phases, this is beginning to be validated. Nevertheless, if some devices work, there is not really medical validation for the majority of systems.
– Can data logging from these apps or connected devices replace an in-depth sleep exam?
What this can replace is an examination which is done quite frequently in the context of insomnia and phase shifts, actimetry: we record from an actimeter bracelet for two weeks the periods of activity and inactivity. With well-formatted analysis reports, the doctor can use this data to make a balance sheet of actimetry.
– What does it bring to treat sleep problems?
Actimetry does not allow to treat, it allows to make a diagnosis on the type of insomnia: when does it occur, at what time of the night, at the beginning, in the middle or at the end of the night. And this also makes it possible to determine the circadian rhythms of the patient, to know if he is in the morning, in the evening, if he is out of step, in advance or late in phase, for example.
– Does this help guide the diagnosis of a sleep disorder?
Yes, and then we have to be able to use this data to treat these sleep abnormalities. These treatments can in particular be carried out by psychotherapists who offer cognitive-behavioral therapies to treat the most frequent so-called physio-psychological insomnia.
– And for sleep disorders related to other causes?
There are beginning to be connected objects that are validated to detect sleep apnea with a precision that is close to what is obtained with so-called “medical” devices. With two additional advantages: the first is that it is recorded under natural conditions, without discomfort for the patient, and above all that it is recorded over several successive nights with prolonged measurements that are not done for medical diagnoses that are performed over a single night usually for cost reasons. These two advantages should reinforce the use of these devices in the future.
– Some doctors underline the anxiety that this self-monitoring of sleep with connected objects can generate…
This is indeed the case for anxious or hypochondriac patients! Trying to bring them to an optimal sleep determined by an application, this can be anxiety-provoking, therefore producing the opposite effect to that sought which is called orthosomnia. Wanting to guide them towards too perfect a sleep is indeed a risk. But it’s a risk that we find with all well-being devices that offer to become super-normal individuals!
– What types of devices would you recommend for those who suffer from sleep disorders?
We know that to detect sleep apnea syndrome there are devices that work well. For the monitoring of insomniacs, there are connected devices which should be able, provided that we manage to obtain analysis reports put in a medical format, to be useful to doctors and to make it possible to replace actimetry.
– Your advice on the use of these devices?
The data must always be interpreted with a doctor to be sure that there is no error in their analysis and to avoid the problems of orthosomnia of which we have spoken. All devices do not have the same reliability as what is achieved in the laboratory. This use must be indicated and reviewed by a doctor.
.