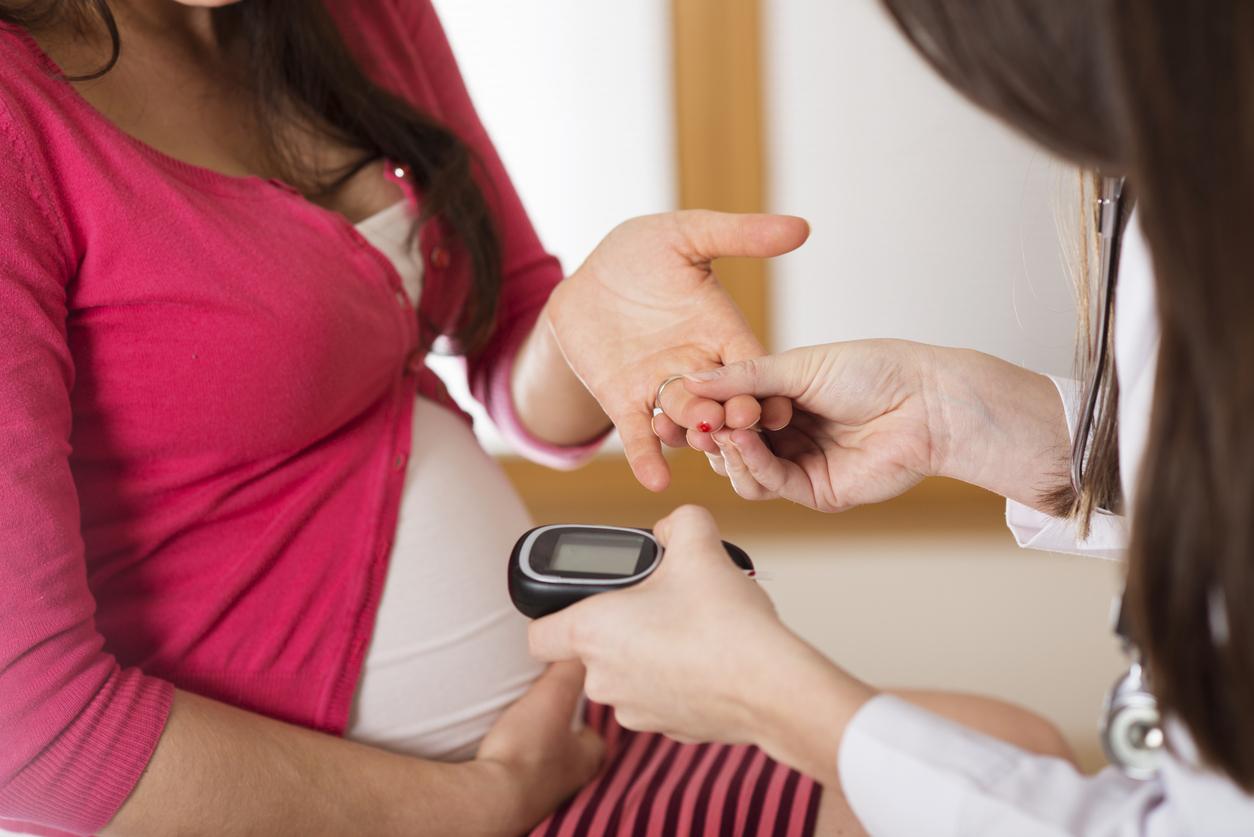
Physical activity is a weapon against diabetes, improving blood sugar levels, fitness and well-being of patients. Anis Nasr, expert sports health educator at Cochin hospital and at the diabetes center, shares his advice and recommendations to ensure a successful and long-term return to exercise.

Anis Nasr, type 1 diabetic, is an expert sports health educator at Cochin hospital and at the diabetes center. He uses his experience and knowledge to organize physical activity workshops aimed at therapeutic patient education. These are designed to (re)instill a taste for exercise, but above all the tools to become independent in its practice. The specialist discusses the importance of physical activity and a healthy lifestyle in the fight against diabetes.
Why Doctor: Why is physical activity essential for diabetics?
Anis Nasr : For all chronic pathologies, physical activity is a non-drug and therapeutic treatment. In diabetics in particular, it helps improve quality of life, promote weight loss and preventively protect organs that can be impacted by blood sugar.
When I establish the physical activity program with the patient, we base it, among other things, on the organs affected by diabetes and the activities that can protect them. For example, this disease can cause a loss of muscle mass in some people, and doing muscle strengthening will stabilize it. Furthermore, this increases muscle glycogen reserves (complex carbohydrates stored in the muscles), and thus by domino effect insulin sensitivity. If it is the heart that is impacted, you should favor aerobic activities such as zumba, swimming, cycling, walking or dancing. Aerobics encompasses all sports in which oxygen is used as energy. It improves the patient’s cardio-respiratory functions, so the heart will be better protected.
Of course, physical activity must be coupled with health and diet advice to help regulate blood sugar and weight. We have sometimes seen patients have reversible diabetes thanks to a balanced diet and regular physical activity. On the other hand, if they do not continue them alone in their daily life, diabetes can return.
Another benefit: when we do sport, we secrete pleasure hormones. Thus, there is also an improvement in psychological health or even self-confidence. We feel better, even a different person. This really has a huge impact on the patient.
Fear of hypoglycemia: “this is truly the first obstacle to exercise”
Although the benefits of physical activity are known, some diabetics have difficulty integrating it into their daily lives. What are their obstacles?
During my workshops, diabetics often talk about the fear of having hypoglycemia during their physical activity sessions. This is truly the first obstacle to exercise for them. The other is the representation of physical activity itself. Patients tend to project themselves into what they have known in the past. Their selective memory will highlight all the bad times they had in sports lessons or the negative representations they have of them. For example, the famous rope climb in college.
But in reality, physical activity is not linked to the search for performance like “sport”. It’s about being as less sedentary as possible and moving through all the gestures of everyday life. In my workshops, I teach them how to improve their quality of life by being active in a way adapted to their health and personal capacity. It also has to be therapeutic. That is to say that we must see the benefit of this energy expenditure, of this movement, in the management of blood sugar levels on a daily basis.
Lack of motivation, fatigue, laziness can be another problem. This is why I build with them a program adapted to their professional and personal lives. We really base ourselves on everything: their treatment, associated pathologies, their life, their tastes…
What advice would you give to diabetics to overcome these obstacles?
For patients who are afraid of hypoglycemia, we first need to know where it comes from: is it linked to poor adaptation of the treatment? Does this come from bad practice? For example, one of my patients who had a multi-injection treatment did not know her carbohydrate and insulin ratios. As soon as she ingested a food, the doses of insulin she took were too high and she had hypoglycemia when she went for a walk or did a leisure activity like gardening. When her treatment was better tailored to her needs, she was able to exercise without fear.
In addition, you should know that when you do physical activity, there is energy expenditure. When it is moderate, it will lower glucose levels. On the other hand, when it is intense, the latter climbs. But, the body’s response is different for each patient. You must therefore identify which one causes your blood sugar to rise and which one which lowers your blood sugar levels. For example, the patient may say to himself: I am more of a person who walks than one who does weight training. I recommend making a table to note the effects of different activities on your blood sugar levels in order to better understand it.
Diabetics can also see the evolution of their blood sugar thanks to regular or permanent glucose monitoring with a blood sugar sensor like the Freestyle Libre 2 during meals… but also during and after physical activity. We must not forget what happens afterwards. This is where blood sugar levels are likely to drop or spike.
However, patients may have difficulty explaining or using these numbers effectively. This is why you should not hesitate to ask for help, from your doctor or from the Diabetes and Obesity Centers near you. Workshops like mine help you return to work and acquire an independent practice. They support diabetics so that they understand their illness and find the program best suited to them. There is teamwork with the doctors who adapt the dosages of the treatment, the sports and health educators like me who define the frequency, the types of exercise and the number of series to do or the dietician who will set up the diet to follow and adapt it to the change in lifestyle. The advice is put in place with them, because it is the patient who is at the center of the change. It is up to him to decide if he wants or can do things. We don’t force, because if we force: he will say yes to please, but the motivation will not be there and he will give up.
“We must be aware that loss of motivation can occur”
And how to stay motivated?
Motivation can come from several factors. It can be intrinsic, that is to say the patient is motivated because he wants to improve his quality of life and his health. It’s often there at the beginning. But it is difficult to maintain in the long term. We then tend to attach ourselves to extrinsic motivation: for example children, family, spouse. Caregivers have an important role in resuming and maintaining physical activity. Encouragement helps motivate the person and bring them back or keep them on track.
To nourish motivation, it is also important to focus on the improvements obtained through regular practice: better quality of life, well-being, etc. Of course, from time to time, there is a drop in motivation and attendance. , but it is part of the patient journey. You must be aware that loss of motivation can occur. This can come from many things: family aspect (divorce, death, argument), work (stress, loss, etc.). It is then necessary to remobilize the memories concerning the benefits that occurred so that he can take action again.
“Exercises adapted to unbalanced diabetes through pétanque”
Are certain activities recommended for getting back into physical activity?
The simplest things are often the best. Brisk walking is recommended. It is good for the heart, for breathing, for the upper and lower limbs (because there is flexion of the hips and knees, ankles). The patient can regulate his blood sugar levels by walking. The advantage is that we get results very quickly. The disadvantage: you have to change the programs regularly (every three months) because the body gets used to it and not much happens if you keep the same rhythm.
You can also do combined. That is to say muscular work to increase muscle mass then aerobic work to regulate blood sugar and try to lower it. Physical activity is truly tailored to each person. It is particularly recommended for type 2 diabetics who often have metabolic problems (obesity) or other pathologies such as osteoarthritis, tendonitis, cardiovascular diseases, etc.
During our workshops, we pay attention to setting up a preventive sport adapted to the person, their treatment of course, but also their pleasure. For example, I had a patient who didn’t like sporting activity, but he loved pétanque. So, we implemented exercises adapted to his unbalanced diabetes through pétanque. When he played, it was always him who went to get the jack, he went back and forth to count the points. When he threw his balls, he had to do a hip flexion to work the squats. He makes movements with the balls to work the biceps and triceps, shoulders, back muscles. And he had to do this program every day. And he held on thanks to this daily pleasure practice.
Our physical activity programs for diabetics are long-term and multi-disciplinary follow-up. Indeed, if we talk about treatment, we have to talk about food, if we talk about food, we talk about well-being. Above all, we must adapt to the needs of each diabetic person and teach them to stay active even without the group.