Thanks to the decoding of the genome, it would be possible to prevent certain frequent diseases. Researchers argue in favor of systematizing this practice.

- More frequent genetic screening would reduce frequent diseases such as cancer or diabetes by 10 to 50%
- Personalized medicine would then allow preventive measures. In the case of diabetes, the savings vary from 96 to 534 billion dollars.
- The authors of this modeling argue in favor of a more incentive-based health policy, in particular through better reimbursement
Personalized medicine is a source of savings for the health system. They even amount to billions, across the United States. Five American researchers have modeled the impact of the wider use of DNA testing on public health. In the Lancet, they argue in favor of a financial incentive policy that boosts the use of precision predictive medicine.
10 to 50% fewer cancers
The factors of genetic predisposition to various diseases are increasingly identified. Screening tests are also starting to emerge on the market. It is this observation that motivated researchers to model the impact of more frequent use of precision medicine. For that, they explain, it would be necessary to adapt the treatments to the vulnerabilities of each one to certain diseases, to target the people at high risk and those who would derive the most benefits from the prevention.
Personalized medicine will mainly help reduce the incidence of 6 diseases: cancer, diabetes, cardiovascular disease, high blood pressure, lung disease and stroke. Between 2012 and 2060, they are expected to decline by 10 to 50% according to estimates. In terms of health spending, for diabetes for example, the low end translates into savings of $ 96 billion. The main gain is on the side of healthy life expectancy after 50 years.
Up to 607 billion savings
Cardiovascular diseases will be best prevented by the wider use of precision medicine. If they fall 50%, the United States will spend $ 607 billion less. “Interventions targeted at reducing cardiovascular disease would bring the greatest social benefits, as they are very common and have a major impact on life expectancy,” explains Dr Victor Dzau, first author. Other diseases, such as stroke or lung disease, are less prevalent and offer less opportunity to extend healthy life expectancy by reducing their incidence. “
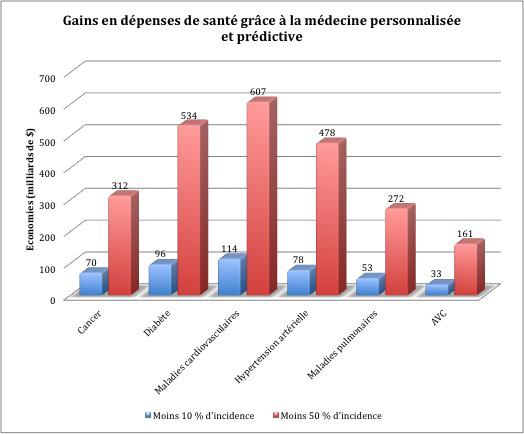
Source: The Lancet
Repay to democratize
If predictive medicine is to be cutting-edge, treatments are not forced to evolve, say the researchers. “In our scenario, the innovation of precision personalized medicine helps identify the number of patients for whom an intervention is most beneficial,” they write. Thus, physical activity for the prevention of diabetes could be prescribed to those who would be the most observant.
On paper, the prospect is enticing. But too few financial incentives in this direction are offered, deplore the authors of this model. Both the public and private sectors suffer from a short or medium term vision. “The current reimbursement rate by the US health care system is characterized by short-term budgetary pressures; it does not encourage the development of preventive, personalized and precise medical interventions, deplores Dr Dzau. He favors treatments that generate less overall wealth, but provide the best return on investment in the short term. To make a difference, reimbursement should be based on the value of the tests, not their actual cost.
.