Mice with Duchenne muscular dystrophy recovered more than 20% of muscle strength thanks to a traditional oral antidiabetic, metformin.
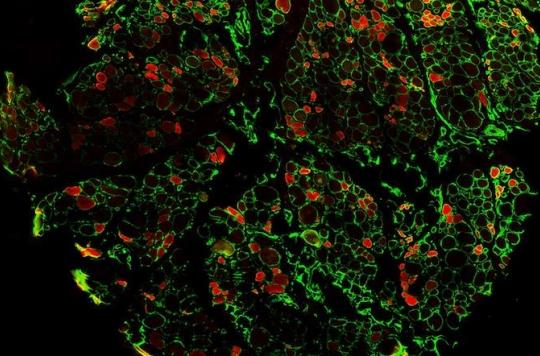
Mice suffering from Duchenne muscular dystrophy and treated for three weeks with Metformin, an old oral antidiabetic, see the quality of their muscles improve, with a gain in muscle strength.
This result is achieved by stopping the pathological process of progressive replacement of muscle fibers by fibrous scar tissue, a phenomenon characteristic of this disease. Indeed, metformin is also a pharmacological activator of AMPK, a molecule regulating the inflammatory process triggered by certain white blood cells in the disease: the pro-inflammatory macrophages.
The destruction of muscle fibers and the formation of fibrous scar tissue decrease respectively -56% and -23%, and especially the regeneration of muscle fibers would increase by 38%. At the end of the treatment, the force measured at the level of the muscles surrounding the tibia of these animals would increase by more than 20%. These results, from the work of Inserm Unit 1217 of the NeuroMyoGene Institute, at the University Claude Bernard Lyon 1, are published in the journal Cell Reports.
A genetic myopathy
Degenerative myopathies such as Duchenne muscular dystrophy (DMD) are currently incurable and are, ultimately, cell and gene therapies under development. These muscular dystrophies of genetic origin are characterized by repeated lesions of the fibers of the muscles, lesions which trigger permanent cycles of regeneration, associated with chronic inflammation.
This lesion-inflammation-healing process leads over the long term to the disappearance of muscle fibers which are gradually replaced by fibrosis, ie an abnormal increase in non-functional scar tissue (collagen fibers). However, the mechanisms of fibrogenesis are still poorly understood in this context.
Block pro-inflammatory macrophages
In this new study, the researchers show that fibrosis in the muscles of patients and mice with Duchenne muscular dystrophy is associated with the presence of specific immune cells (certain white blood cells), the “pro-inflammatory macrophages”. These macrophages overexpress a protein which is necessary for the secretion of a growth factor (TGFβ), the main cause of fibrosis: once released and activated in the cellular environment, TGFβ stimulates the production of collagen by the fibroblasts.
This excessive formation of fibrous tissue can however be limited by the activation of a regulator normally present in macrophages, AMP kinase (AMPK), which decreases their pro-inflammatory state. The activation of AMPK, by decreasing the expression of the protein necessary for the secretion of TGFβ, therefore limits fibrosis. However, it turns out that metformin, an old oral antidiabetic commonly used in type 2 diabetes, is a pharmacological activator of AMPK.
Validation in mice
Mice treated for three weeks with Metformin see their AMPK stimulated, inflammation and the formation of fibrosis regress, and the quality of their muscles improve, with a gain in muscle strength. The inflammatory process in the muscle seems identical in mice and humans, but Metformin is a drug that is very easily available and has already been used in humans for type 2 diabetes.
The researchers are now focusing on dissecting the great heterogeneity of the macrophage populations in this muscle disease, in order to identify the “bad” pro-fibrotic subpopulations from the “good” repairing subpopulations which, in turn, help to muscle regeneration.
promises and work
This work shows that pharmacological approaches targeting inflammation and the resulting fibrosis could be considered in humans to improve muscle condition in Duchenne muscular dystrophy.
Metformin is already available, as it is widely used in type 2 diabetes, but it is not yet time to prescribe it in Duchenne muscular dystrophy. There is still work to be done and it is necessary in particular to determine the useful dose in this muscular dystrophy and to know when its use has the most interest in the context of cell or gene therapies.
The researchers recommend possibly using it initially to reduce the inflammatory state of the muscles of the patients, in order to increase the effectiveness of cell or gene therapies, which alone will make it possible to cure the patients.
.

















