In chronic infection, viral replication is prolonged and the opportunities for the virus to mutate increase. These mutations lead to the appearance of variants which are of concern and which could defeat the effectiveness of vaccines, as suggested by a study on the AstraZeneca vaccine and the South African variant.
- In France, one in five infected people is infected with a variant (British, Brazilian or South African).
- The variants develop in patients with long Covid, in whom the virus has time to adapt against the immune system and treatments.
- South Africa has stopped using the AstraZeneca vaccine after the publication of results showing its ineffectiveness against the variant discovered on its territory.
As of February 3, the variants represent in France more than one new case of coronavirus detected in five (21.3%), according to a document submitted on February 5 by Health Insurance to medical biology laboratories. A figure that should rise further since many specialists believe that the British variant, the most present on our territory, could become the majority by March. The South African variant circulates mainly in the east of France where cases have been detected in Metz and in the territory of Belfort. Only four cases of the Brazilian variant have been discovered, announced the Minister of Health Olivier Véran last Thursday during a press conference. The spread of these variants worries the government, which has put in place new measures to strengthen the health protocol this Sunday, February 7.
A mutation on the spike protein of the virus
But how do variants develop and why do they raise fears that vaccines will be less effective? British researchers from the University of Cambridge observed the mutations of the virus in the laboratory to better understand them. The team of virologists suggests that new mutations could arise in the event of chronic infection because of the treatment taken over a prolonged period which offers the virus multiple opportunities for evolution. Particularly when treating immunocompromised patients where prolonged viral replication increases the opportunities for the virus to mutate, they observed during follow-up of an immunocompromised patient treated with convalescent plasma.
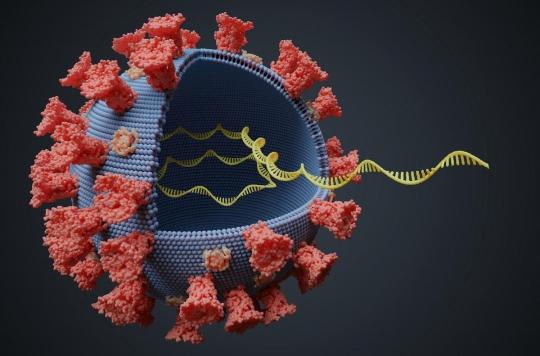
SARS-CoV-2 is a low mutation beta coronavirus. Its RNA, i.e. its genetic code, is made up of a series of nucleotides, chemical structures represented by the letters A, C, G and U. When it replicates, the code of the virus can be wrong transcribed, leading to mutations. Of these possible mutations, those that affect the structure of the spike protein, the one that sits on the surface of the virus and gives it its characteristic crown-like shape, are of most concern. It is this protein that is used by the virus to attach to the ACE2 receptor on the surface of host cells to penetrate and infect them. Most of the vaccines currently in use or being tested target this spike protein and new mutations are feared as it could affect the efficacy of these vaccines.
Mutations that adapt to treatment
For the first time, the researchers, who published their results on February 5 in the journal Nature, documented how these mutations arose in a hospitalized patient. They identified a particular variant of the virus that includes significant changes that appear to make it more infectious: the deletion of certain amino acids, ΔH69/ΔV70, in part of the peak protein. The patient was diagnosed with a rare type of B-cell non-Hodgkin’s lymphoma (NHL), and recently received chemotherapy, weakening his immune system. After his admission, he received a number of treatments, including the antiviral drug remdesivir and convalescent plasma. His condition deteriorated and he was admitted to the intensive care unit only to die. During his hospitalization, 23 viral samples, mainly from his nose and throat, were analyzed and sequenced.
The researchers were able to observe the mutation of the virus genome. They found that after the first administrations of the treatments, a radical change took place in the viral population with the emergence of a variant that had become dominant. This one carried deletions, it is a loss of the genetic material, ΔH69/ΔV70, as well as a mutation in the spike protein known as D796H. While the variant appeared to disappear at first, it reappeared upon administration of the third cycle of remdesivir and plasma therapy. “What we observed was competition between different variants of the virus and we believe this competition was triggered by the convalescent plasma therapy”, wrote the researchers.
Subsequently, the researchers created and tested a synthetic version of the virus with these same variants, the ΔH69/ΔV70 deletions and the D796H mutations both individually and in combination. The combined mutations made the virus less susceptible to neutralization by convalescent plasma, demonstrating that the mutations allow the virus to adapt to escape immune pressure. The ΔH69/ΔV70 deletion made the virus twice as infectious as the starting strain.
The effectiveness of the vaccines in question
These mutations raise fears of the virus’ ability to adapt, which could affect the effectiveness of vaccines. “Since vaccines and therapies target the spike protein, which we see mutating in our patient, our study raises the risk that the virus might mutate in ways that thwart vaccines.conclude the researchers. Finally, this mutation phenomenon unlikely to occur in patients with well-functioning immune systems highlights the need for monitoring when treating immunocompromised patients, where prolonged viral replication increases the opportunity for the virus to mutate..”
These fears seem to be confirmed with the South African variant which seems to reduce the effectiveness of the AstraZeneca vaccine. Revealed on Sunday, a South African study, conducted by the University of the Witwatersrand in Johannesburg but not yet confirmed by countries, believes that the British vaccine offers a “limited protection against moderate forms of the disease”. Results which are also confirmed for the Johnson & Johnson and Novavax vaccine candidates. “The first results seem to confirm that the virus mutation detected in South Africa can be transmitted to the already vaccinated population”, is it written in a press release. The country has also announced that it has stopped using the AstraZeneca vaccine on its population.
The study was carried out on 2,000 volunteers aged 31 on average. The results therefore do not make it possible to determine the effectiveness of the vaccine against severe forms of the disease, hospitalizations and deaths “because the target population was at low risk”, judges the University of the Witwatersrand. “We believe that our vaccine will still protect against severe forms of the disease, as the neutralizing antibody activity is similar to that of other Covid-19 vaccines that have been shown to be effective against severe forms, particularly when doses are spaced 8 to 12 weeks apart”, reacted a spokesperson for AstraZeneca to AFP. Separately, Sarah Gilbert, who is leading vaccine development at Oxford University, told the BBC on Sunday morning that “a version (of the Oxford/AstraZeneca vaccine) with the sequence of the South African variant is in preparation” and hoped for the fall.

.