Psoriasis does not only affect the body of people with it. It also affects the mind. It is a major risk factor for depression.

This is commonly called the double penalty. People with psoriasis don’t just suffer physically. This chronic skin disease also carries a psychological burden. It is even a major risk factor for depression, according to a study published in the JAMA Dermatology.
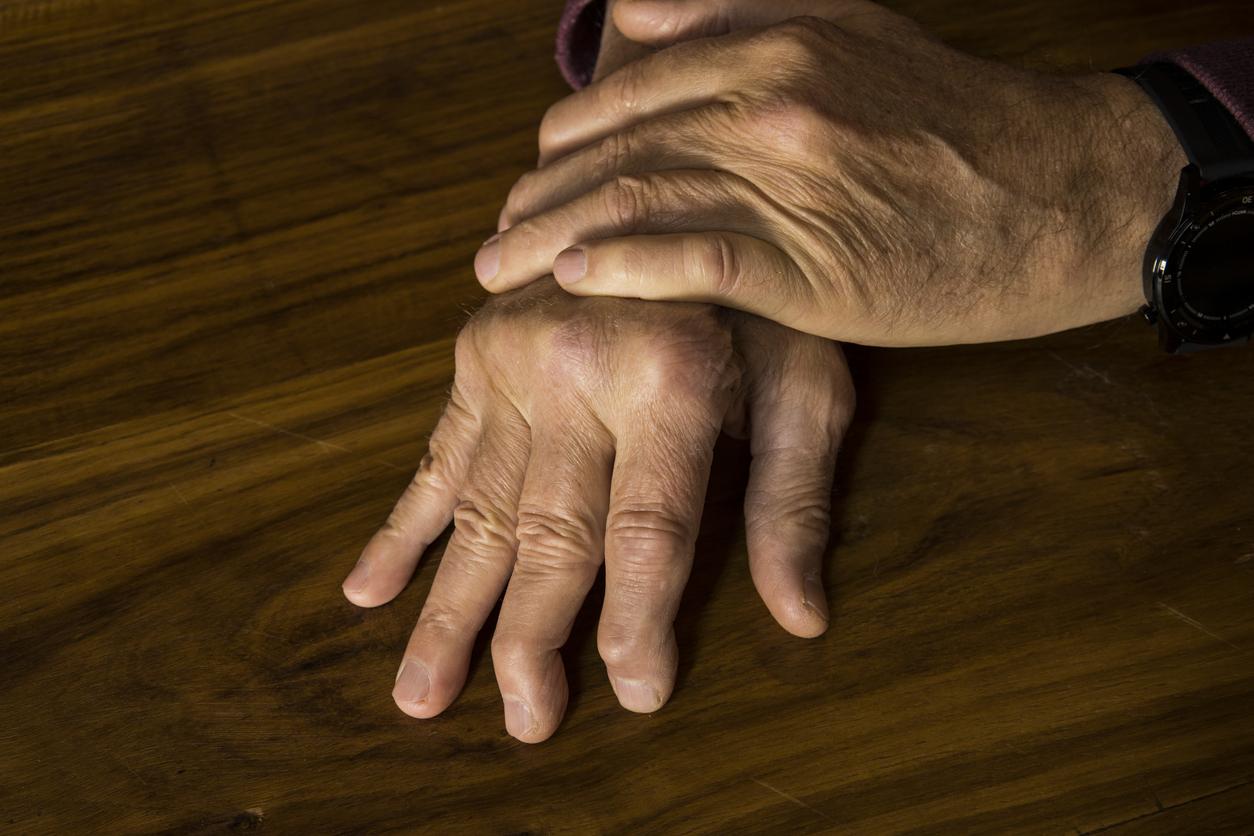
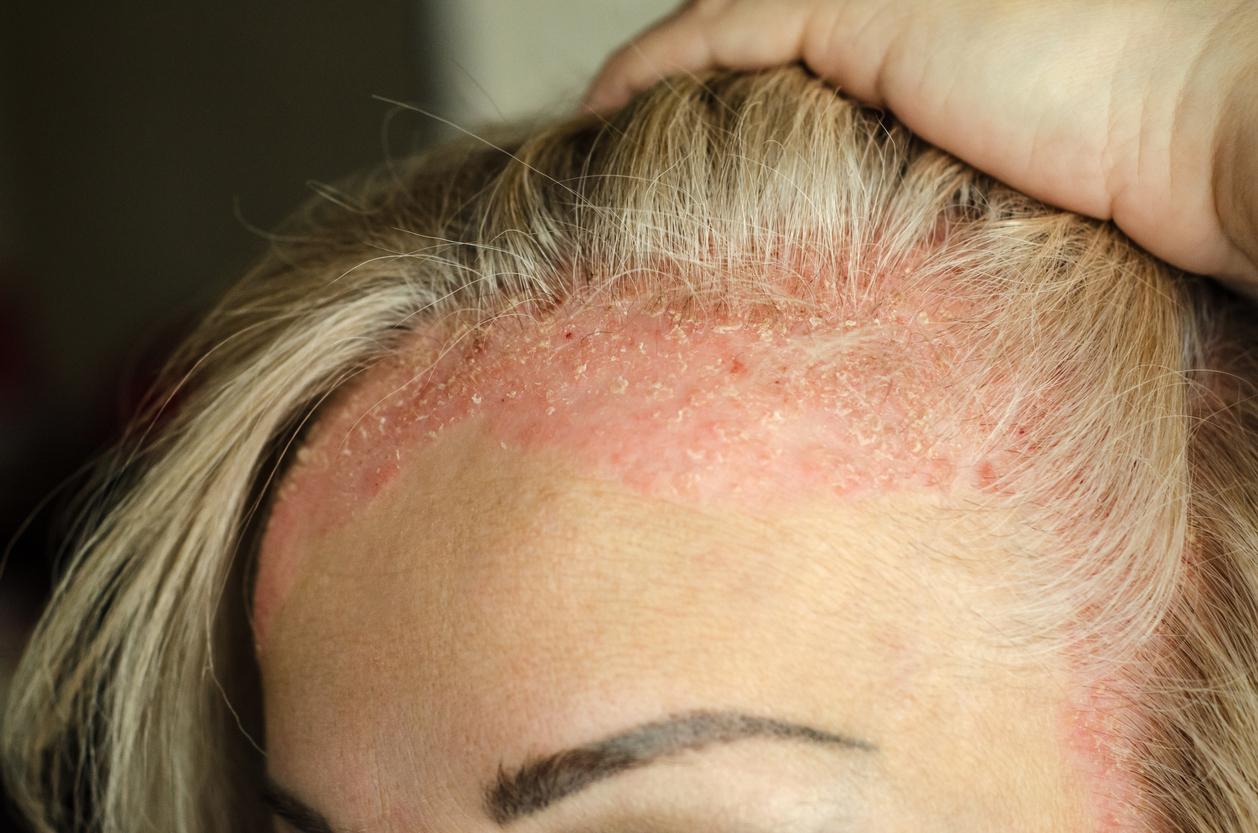
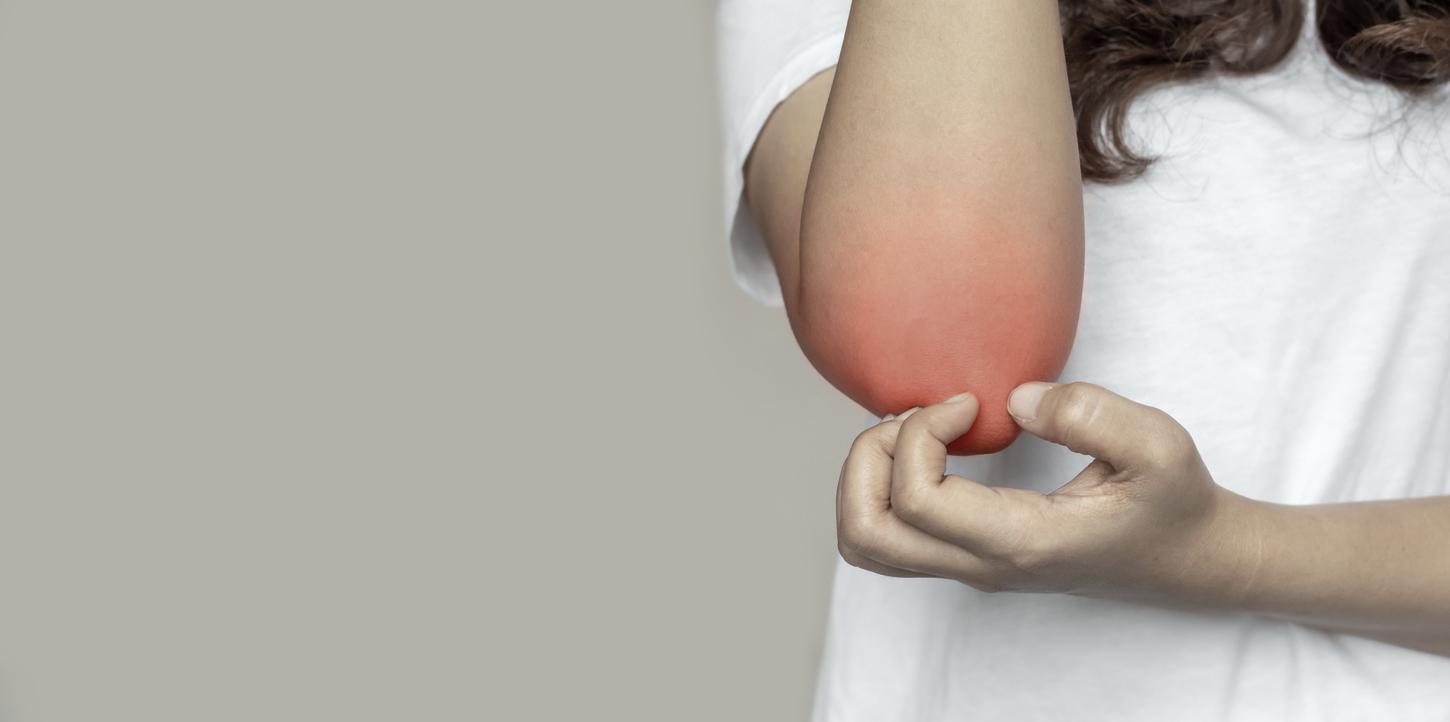
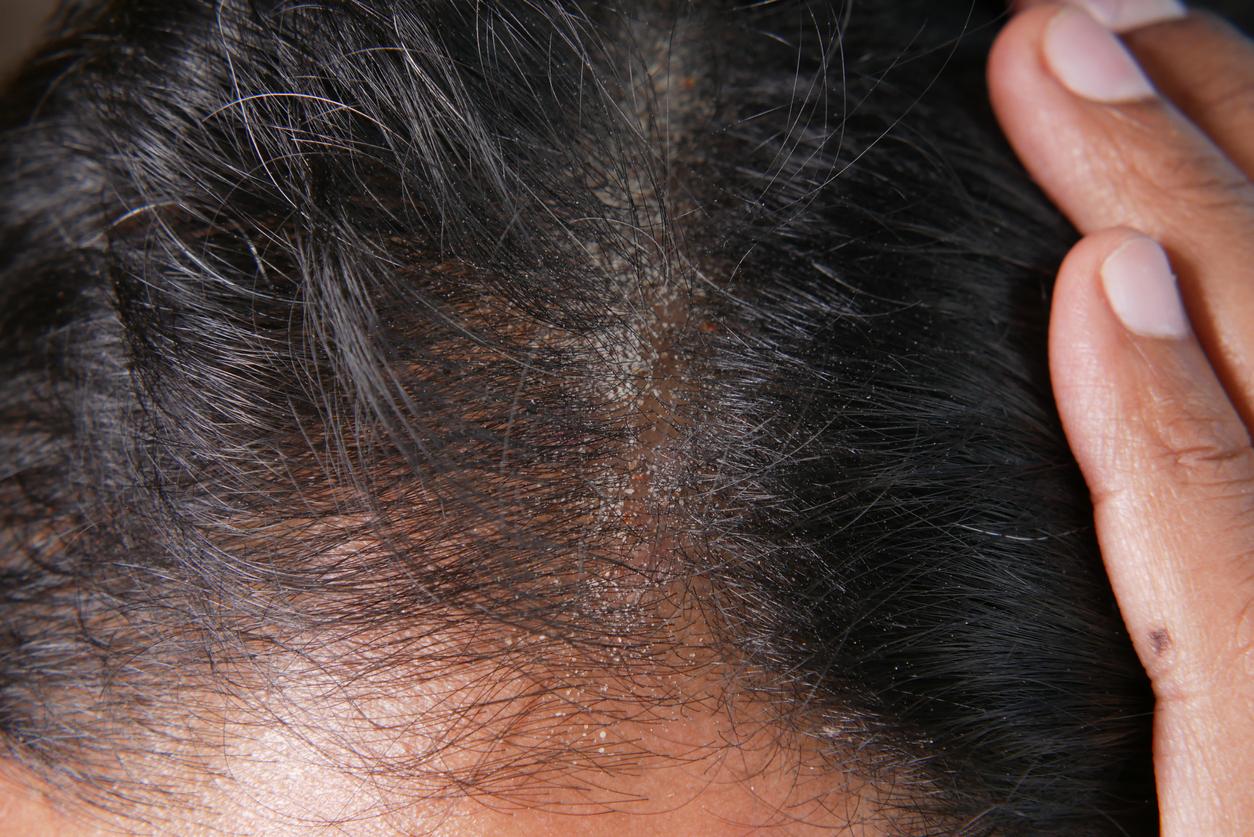
Red patches covered with scabs: Psoriasis is an unpleasant-looking disease. It is even often taken for a lack of hygiene by the general public. These discriminations directly impact the mental health of patients. A team from the New York University School of Medicine (United States) demonstrated this by monitoring 12,382 people representative of the American population.

Perception affects the mind
2.8% of the participants had psoriasis, and 7.8% suffered from depression. The proportion of people with depression is higher in psoriatic patients: 16.5% show symptoms. They are also slightly more likely to have thoughts of suicide. “In this study, psoriasis was the only disease significantly associated with suicidal ideation, and the majority attributed them directly to their psoriasis,” say the authors.
The occurrence of depression does not depend on the symptoms themselves, but rather on how sufferers perceive them. “The psychological burden of psoriasis may be more closely related to patients’ perception of social reaction to their appearance than to the objective severity of the disease,” they write. Which could explain why depression has more impact on the quality of life of psoriatic participants. 24% of them consider that their ill-being causes a daily functional limitation. In physically healthy patients, only 15% thought the same.
Monoclonal antibody reduces symptoms
A very effective treatment for psoriasis has just delivered its results. Two phase 3 clinical trials, published in the New England Journal of Medicine, concludes that the brodalumab monoclonal antibody provides a 100% reduction in symptoms. This drug blocks a protein involved in the immune reaction that causes skin reactions, interleukin 17. “The treatment was so effective that many patients no longer had a trace of psoriasis on their body,” says Mark Lebowhl with satisfaction. , co-author of the study.
At 12 weeks of treatment, 44% of patients on brodalumab had their symptoms reduced by 100% – compared to 22% of participants on ustekinumab, which is the standard treatment. In the second study, a gap also widened between the two groups, and a majority managed to reduce symptoms by 75% – which was the main objective.
Brodalumab is therefore more effective, but with as many side effects as ustekinumab. During the study, the researchers counted respiratory infections, joint pain, a drop in the number of white blood cells, inflammation of the mucous membranes and cases of yeast infection. Two participants committed suicide, one during the randomization phase, the other when brodalumab was extended to all. “Regardless of treatment, psoriatic patients are at increased risk for depression, anxiety and suicidal ideation. No causality between brodalumab and these events has been established, ”said a statement.
.