Although it is particularly difficult to diagnose osteoporosis, it is possible to detect it by bone densitometry. Reliable, fast, little irradiating, this examination remains however very little requested. The reason: support that is too limited.

- Densitometry is one of the most reliable ways to diagnose osteoporosis
- It is better to wait 60 years to do this examination
- Densitometry is only covered by health insurance for people said to be at risk of osteoporosis
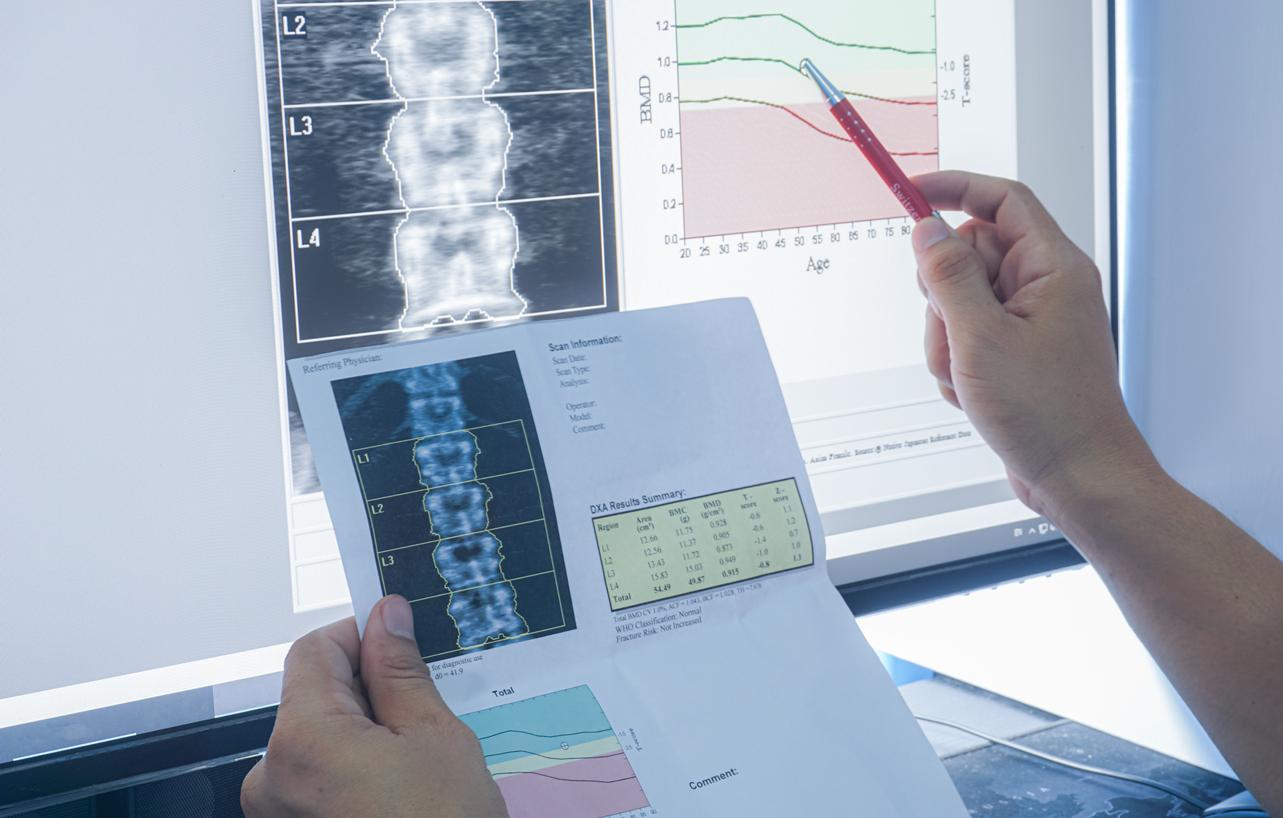
So-called “silent” bone disease, osteoporosis is particularly difficult to diagnose. However, an examination can detect it; this is bone densitometry, which determines the presence of any bone fragility. “It is a simple, perfectly reliable examination, which does not require fasting, which does not require injections, and which provides extremely precise information”explains to why doctor Professor Bernard Cortet, rheumatologist at the University Hospital of Lille.
Concretely, the bone densitometry lasts only a few minutes. It delivers X-rays – while being less irradiating than a scanner or a chest X-ray – in order to measure the calcium content of the bones in the vertebrae and hip, two potential areas of fracture and fragility.
“The amount of bone is a very important element in predicting bone strength”
“It’s a test that measures the amount of bonedevelops the rheumatologist. We have no information on the quality of bone tissue, but we know that this quantity of bone is a very important element in predicting bone strength, and therefore in predicting the risk of fracture.”. The latter is frequent in certain conditions: it rises to 40% in women over 50 years of age.
However, it is advisable to wait until you are almost 60 years old to do a bone densitometry, rather than carrying out the examination shortly after menopause. In question: the bone loss that occurs in the 5 to 10 years following this menopause. Since men are less exposed than women to osteoporosis, it is recommended that they be screened later.
A review of the scope of reimbursement still too limited
One problem, however: in France, bone densitometry is not reimbursed only under certain conditions. Thus, care only concerns postmenopausal women with risk factors – such as a history of fracture of the femoral neck without trauma in one of the parents – as well as people, regardless of their sex, with a pathology or treatment potentially inducing osteoporosis, or subject to a history of fracture without major trauma diagnosed during an X-ray.
“The figures show that it does not work since there are fewer and fewer densitometric examinations requested, which goes completely against the data since there are more and more fractures”, regrets Professor Bernard Cortet. With the GRIO (Osteoporosis Research and Information Group)of which he is a member, the healthcare professional requests an extension of the scope of reimbursement for bone densitometry.
He recommends sticking to an age threshold, set at around 60 to 65 years. “By certainly favoring women, since they are more prone to osteoporosis, but why not in men, especially in those who have risk factors beyond 70 years old”continues the rheumatologist.
“We are not going to say that we only monitor this tool”
Apart from the reimbursement conditions, bone densitometry has a limit. Given that a certain number of fractures which occur in the absence of bone fragility are accompanied by a lowering of bone density which may prove to be consequent, the examination could detect, wrongly, osteoporosis.
“We are not going to make a decision, say that we are implementing a treatment or that we are monitoring only on this toolassures the doctor. Obviously, in parallel, we must question the patient, know her risk factors, find out if she consumes alcoholic beverages in excess, if she has taken cortisone, if she has had breast cancer which has justified treatment. particular…”. In short, bone densitometry is a reliable screening tool, when it is part of a more global follow-up.
.