You have surely happened to grind your skin, to empty blackheads, pierce pimples, clear a scab… There is nothing very original about it. But in some people, touching the skin can become obsessive, to the point of injury. This disorder is called “dermatillomania”. The MSD Manual explains how it manifests and can be treated.
What is it, who is affected?
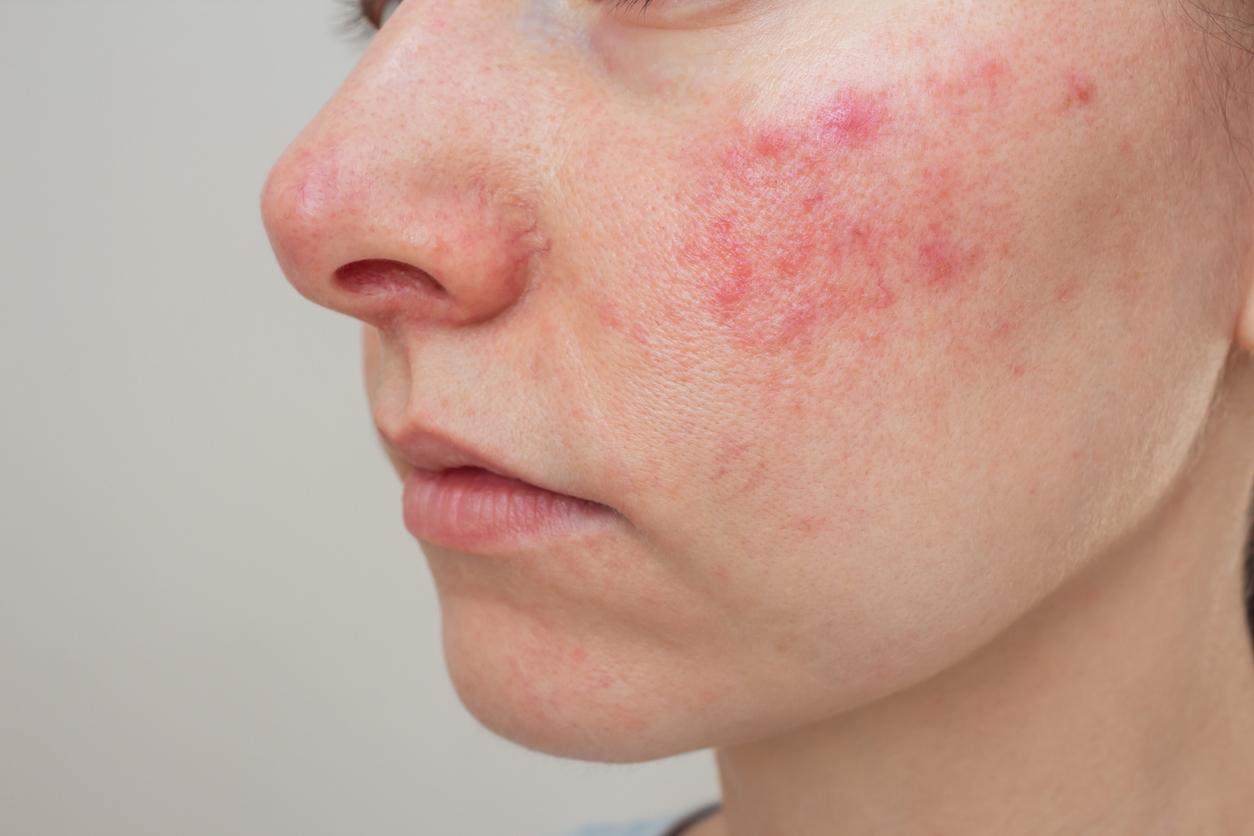
To be a dermatillomaniac is to scratch, rub, pinch, tear or even pierce the skin without necessarily any obvious reason. That is to say that the person affected by this disorder does not necessarily seek to get rid of a defect, he does it compulsively, mere “willpower” is not enough to get rid of this mental illness, which often leaves sufferers helpless and ashamed of their own actions.
Several areas of the body can be affected, and this can change over time. Dermatillomania does not only concern the face, or the back for example. The dermatillomania can do it consciously or automatically, without any particular will.
In a testimonial published on the 20-minute site, Camille, author of “My story with dermatillomania” recounts her crises, which aim to attack the slightest defect on her face, until her skin is damaged. The seizures started in them around 10 or 11 years old, and can last several hours. She also gave birth to an Instagram account, called “peau.ssible”, in which she talks about her illness and what helped her get through it. It also publishes testimonials from people affected and a list of “risky situations” when one is affected.
The disorder mainly concerns women, an estimated 75% of people affected are female. And in general, we find dermatillomania in 1% to 2% of the population. It usually develops in adolescencebut may arise later, notes the MSD manual.
Where does this come from?
“Many dermatillomaniacs also repeatedly pull their hair out, bite their nails, bite the inside of their cheeks, or exhibit other repetitive body-focused behaviors. Some people pick on other people’s skin “, specifies the manual, which associates this disorder with depression or even mental disorders such as TOCS, which are generally also present in dermatillomaniacs.
What are the health risks ?
It is first important to note that dermatillomania reflects a psychological malaise in the affected subject. Then, insofar as the disorder causes wounds, the person is exposed to a risk of bleeding, on the one hand, but alsoinfection, which can lead to blood infection. Dermatillomania causes lesions and develops scars.
How to diagnose and treat dermatillomania?
Several elements make it possible to distinguish dermatillomania from a bad habit. First, the severity of crushing, the presence of lesions on healthy skin can alert. Trying to quit and having a hard time or failing is also a sign. “Doctors diagnose the disorder when a person claws at the skin enough to injure it, if she is trying to stop picking her skin without success, and that she is significantly distressed by her behavior or performs worse because of it,” the MSD manual notes.
Support can be done in two ways. First, via cognitive and behavioral therapy (CBT), useful to help the patient become aware of his act, but also to understand where his disorder comes from, to identify the context responsible for the crises, and finally to get rid of the ocd. A type of antidepressant may also be prescribed in addition.
Sources: MSD Manuals, Instagram, 20 Minutes.
Read also:
- Do I need to see a psychiatrist?
- Trichotillomania: the disorder that pulls your hair out