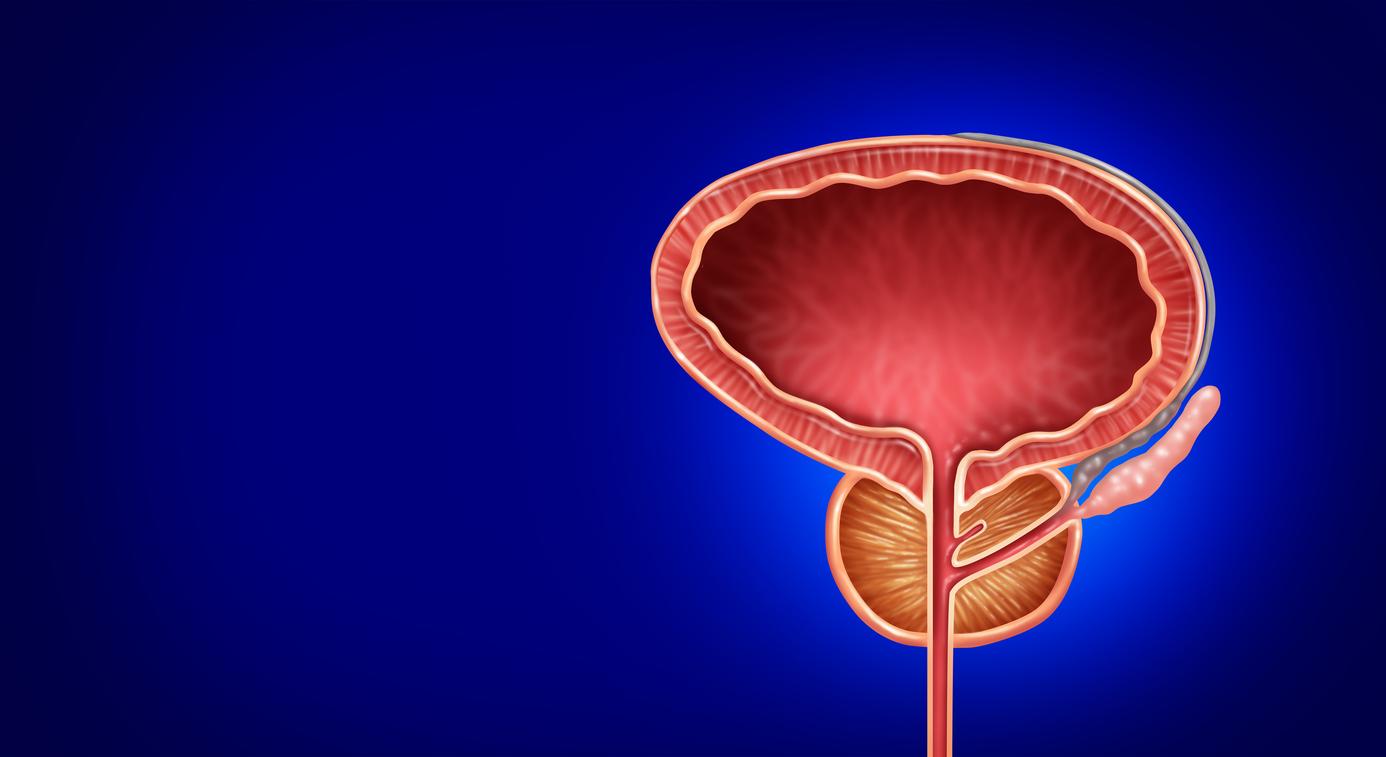
Scanner detection, from a urine sample, of defective cells would be less invasive than cystoscopy and more efficient, especially for low-grade cancers whose cells are very similar to healthy cells. Explanations.
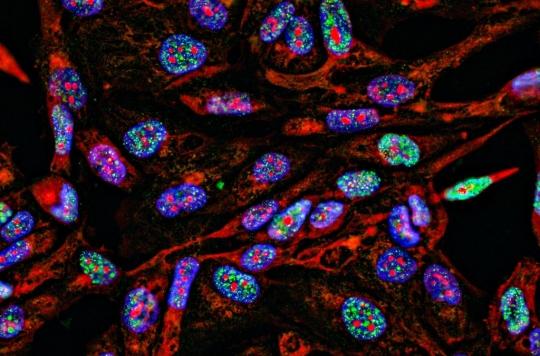
- Chinese researchers claim to have developed a new test for detecting bladder cancer.
- This would detect non-sufferers as well as the current test, but would have better results in recognizing cancers, especially low-grade ones whose abnormal cells visually resemble healthy ones.
And if the detection of bladder cancer was no longer done under a microscope but from a urine sample and using a sequential scanner? This is the bet of Chinese researchers who presented, in the scientific journal Clinical Cancer Research this october 9, the results of their test prototype. This is based on theanalysis of DNA copy number variants (CNV) in cells taken from urine. They assure that it has better results both in sensitivity and specificity than traditional urinary cytology [test qui recherche des cellules anormales dans l’urine au microscope, NDLR] to detect bladder cancer “urothelial carcinoma”, the most common form.
“Urine cytology, which is widely used to screen for bladder cancer, has specificity [probabilité de résultat négatif pour les non-malades, NDLR] high but lacks sensitivity [probabilité du résultat positif chez un malade, NDLR]especially for low-grade cancers [cancer lent dont les cellules anormales ressemblent beaucoup aux saines, NDLR]says Xu Chuan-Liang director of the study and urologist at Changhai Hospital (Shanghai, China). Cystoscopy [examen médical permettant d’étudier la paroi interne de la vessie, NDLR]although more accurate than cytology, is an invasive procedure with additional costs and potential complications for the patient. Therefore, an inexpensive and non-invasive test for the detection and monitoring of bladder cancer is an unmet clinical need.“
Encouraging results
Down with microscopes, make way for new techniques. Chinese scientists have decided to rely on the cancer detection technique called “analysis of DNA copy number variants” (CNV). There to save speed and cost, they decided not to identify each specific genetic alteration, but to assess the overall CNV load via low-coverage whole genome sequencing (LC-WGS). For Viktor Adalsteinsson, associate director of the Gerstner cancer diagnostic center at the Broad Institute (Massachusetts, United States), interviewed by by the National Cancer Institute of the United States this type of sequencing saves a lot of time and money. “ATInstead of loading a single sample onto the sequencer, we load multiple samples so that each receives a small amount of sequencinghe explains. Because it requires only an insignificant amount of sequencing, LC-WGS can be applied to many samples at low cost.“
To prove that the use of CNV via an LC-WGS is more effective than microscopic analysis or medical examination, the Shanghai researchers tested their method on 190 urine samples collected during a clinical trial of observation. They assure that of these 190 samples, 126 contained bladder cancer and 64 did not. However, their method succeeded in detecting people with cancer from others. Then they refined their test to additionally analyze “all autosomal chromosomal changes in exfoliated cells in urine.” On the same data, the Chinese test prototype identified bladder cancer “urothelial carcinoma” with a sensitivity of 82.5% [probabilité du résultat positif chez un malade, NDLR] and a specificity of 96.9% [probabilité de résultat négatif pour les non-malades, NDLR]. Thus the risk of false-negative is 17.5% while that of false-positive is 5.1%.
Better sensitivity
To verify these results, they then tested this prototype test again on a new cohort of 95 patients, including 56 with bladder cancer of the “urothelial carcinoma” type. Compared to microscopic identification, i.e. urinary cytology, this prototype test had better sensitivity [détection des cas mositifs] – 80.4% for the test against 33.9% for the microscope -, and a specificity [détection des non-malades, NDLR] comparable – 94.9% for the prototype versus 100% for the microscope. This difference in the detection of positive cases was widened in the ability to discover the 7 cases of low-grade tumors, whose abnormal cells closely resemble healthy cells. Faced with this configuration, the test prototype had a sensitivity of 71.4% while the microscope found none. According to the researchers, the sensitivity of their test depends on the size of the tumour: the larger it is, the better it detects it. “The relatively lower sensitivity of the test for detecting lower grade or smaller tumors is not unexpected, as these tumors are less likely to have abundant chromosomal alterations.diagnoses Xu Chuan-Liang. Ultimately, we believe our test could help reduce the frequency of cystoscopic medical examinations, but not replace them.“However, the researchers are very hopeful that their prototype test can replace microscopic detection of abnormal cells. This test is again on the test bench to measure what minimum quantity it needs without distorting the results.

.