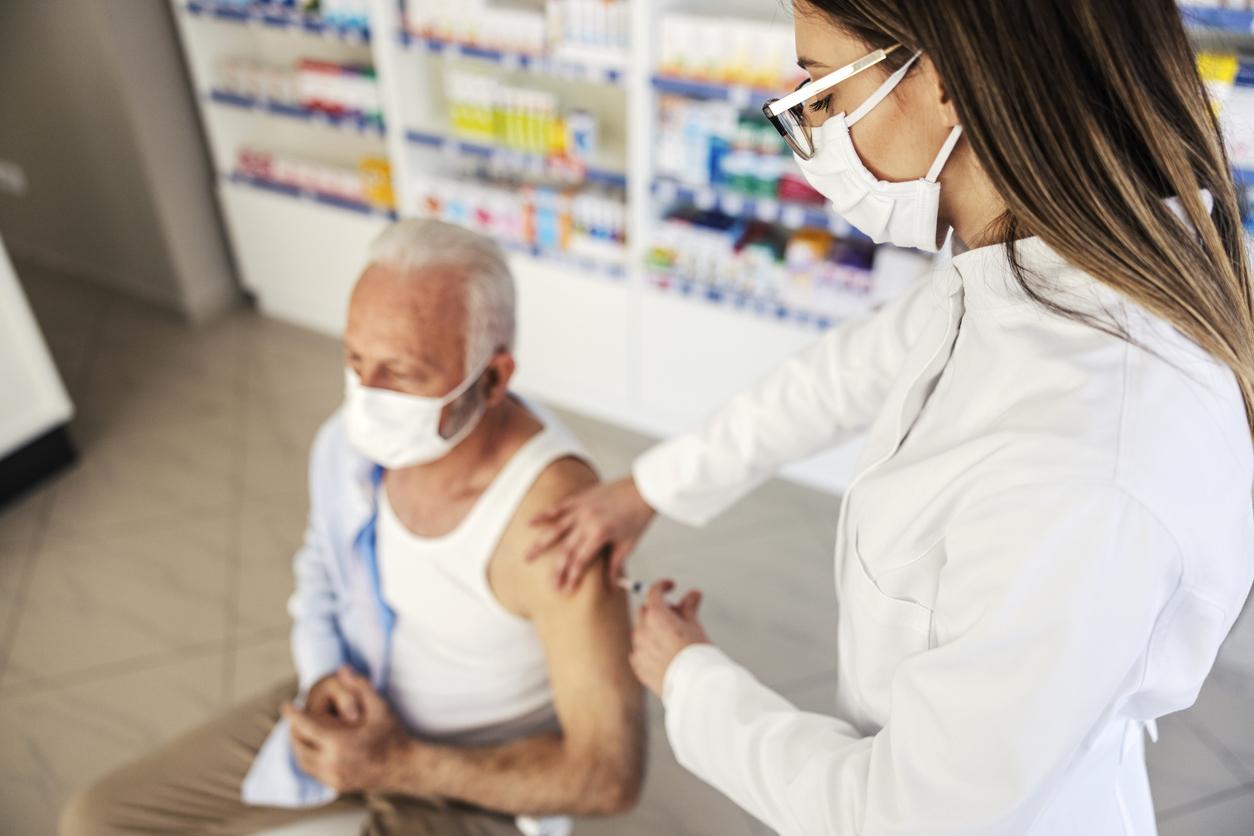
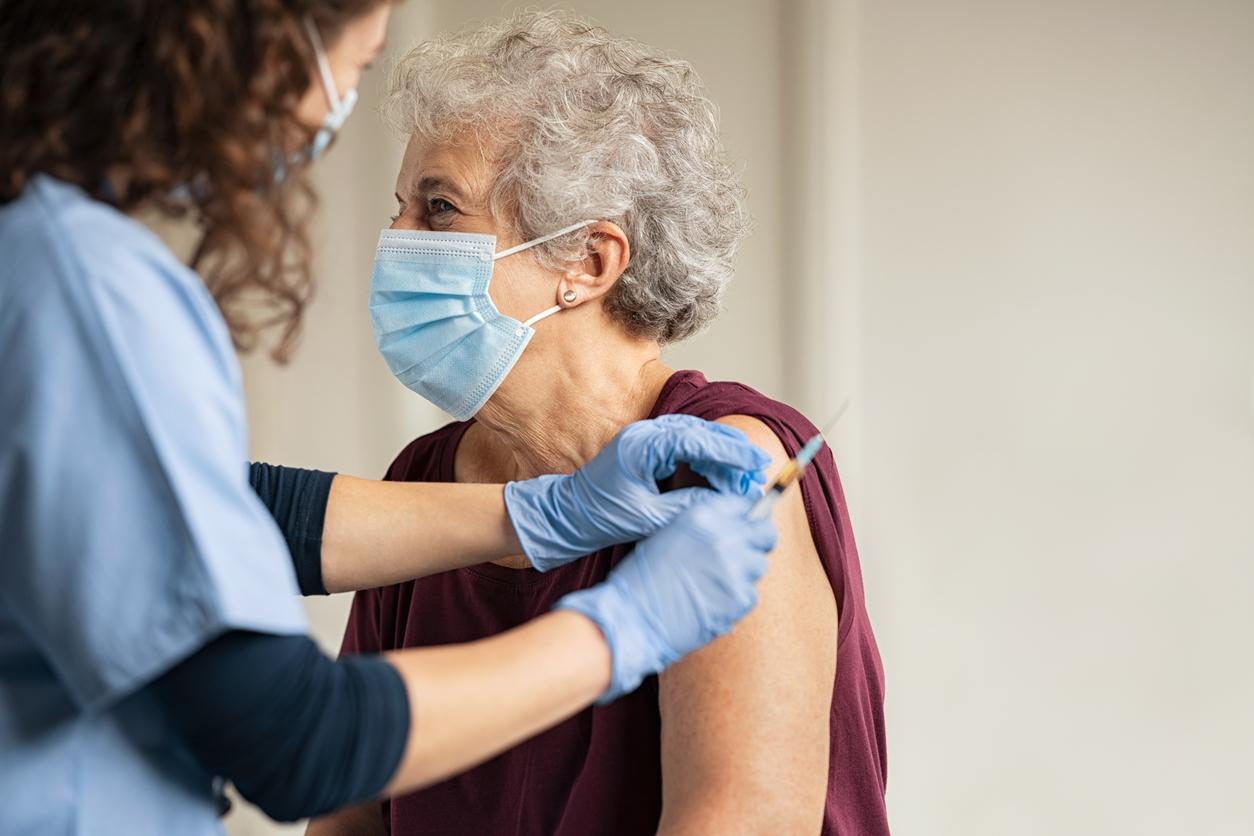
With a stagnant number of beds, a growing elderly population, intensive care units are forced to make admission choices based on age.
“99 years old, septic shock, peritonitis… This is the last patient I saw at Bichat hospital,” recalls Professor Sadek Béloucif, anesthesiologist and former member of the Ethics Committee. In this case, we could have said, it’s over, if I operate, it’s therapeutic relentlessness. In fact, we brought her to the OR because we thought she was just suffering from appendicitis in the old man’s form. This lady spent four days in intensive care and returned home very quickly. For how long, I don’t know. But what I do know is that if her age had led us not to operate on her, we would have fatally condemned her to death. ”
Not all stories end equally well, of course. And Professor Béloucif is careful not to conclude that all the elderly must under all circumstances be hospitalized in an intensive care unit. “But all must, like everyone else, be able to have access to it,” he says. Because the question is not easy to decide. “There is real pressure when entering intensive care services,” says Professor Bertrand Guidet, president of the French language intensive care company (SRLF). There are more and more elderly people while the number of beds is stagnating or even declining. Suddenly, we are facing a double risk: therapeutic relentlessness or loss of luck. “
“A very important selection”
Confronted with the throes of sorting out patients, many resuscitators are carrying out studies to find out if old age is closing doors. A 2006 study clearly shows that age is a discriminating criterion: 36% of those over 85 were refused in intensive care, against 23% of 75-84 years and 12% of 18-44 years. The Ice-Cub study, to be published, carried out on more than 50,000 patients over 80 years of age in 15 hospitals in the Ile-de-France region, agrees. Out of eight people over 80 who go to the emergency room with a potential indication for admission to intensive care, two were proposed by emergency physicians and only one was admitted. “The selection is very important”, comments Professor Guidet. In addition, admission rates ranged from 8 to 40% across departments.
Once the door to the intensive care unit is passed, age continues to weigh in the balance. In any case, this is what seems to demonstrate the study of Dr Edouard Ferrand on decisions to limit or stop active therapies. When asked about the reasons for their decisions, the resuscitators cited age in third place (34%). Two years later, in a similar study, only 3% of caregivers cited age as a decision criterion, but the question was asked differently. This time they had to indicate the major criterion of choice… More prosaically, if there is only one bed left for two patients, the young person has a head start. Why such unequal treatment? In any case, not for medical reasons.
All the resuscitators agree on this point: “Age as such is not, in itself, a factor of poor prognosis”, insists Professor Béloucif. The National Consultative Ethics Committee recalled this in its opinion on “The ethical issues of the budget constraint” at the hospital and even added that “on the contrary, significant advantages can be derived from a rapid intervention allowing the autonomy and mobility of the elderly to be maintained”. If the admission of elderly people to intensive care is debated, it is therefore because the economic pressure is increasing. And the president of the SRLF recognizes that this variable is taken into account. He even goes further by declaring that “we must admit the idea of redistributive justice. If we take in a lot of intensive care patients, this represents a significant cost. And this will necessarily be to the detriment of other services. “
For waiting resuscitation
It remains to be seen how to do this “sorting”. And there, the resuscitators do not want to be the only ones to assume this responsibility. This is why the French-language intensive care company is calling for a social debate on the criteria for admission to the intensive care unit and wishes to issue recommendations in this direction. Already, avenues for reflection have been mapped out. One of them is the use of advance directives. “We have implemented this in Canada,” explains Prof. Hubert Doucet, professor of bioethics at the University of Montreal, “and it has been beneficial.
Patients and families have time to reflect and prepare for difficult decision-making. “(Listen to interview) The other track, which is on the rise in France, is” waiting resuscitation “. The anesthesia and resuscitation teams in Rouen and Dieppe are particularly pleading in favor of this third option after having carried out a study showing that age was in third place among the factors for refusing admission. In their eyes, waiting resuscitation is justified for this population because admitting an elderly person “leads to a more in-depth assessment of the patient, particularly in terms of loss of autonomy or dependence”. It is also necessary that the number of beds be sufficient … “For the moment, we still have the means to provide these waiting resuscitations in most establishments, except in periods of tension like the one we experienced at Christmas. , says Professor Guidet. But the debate is urgent. “By 2050, the number of people over 65 will have tripled.
.